Blodsukker regulerende beslutningsstøtte system
Translated title
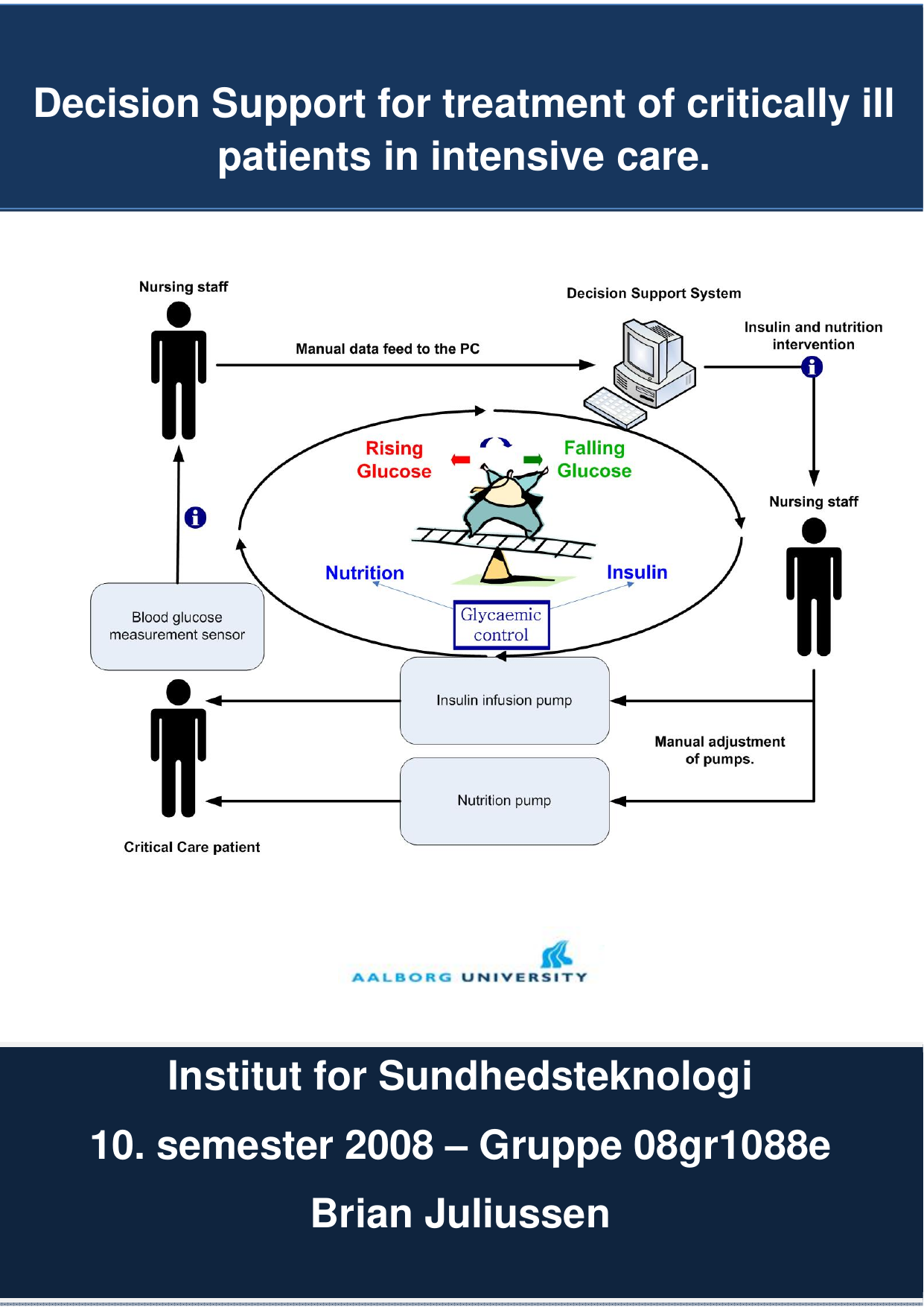
Decision Support for treatment of critically ill patients in intensive care
Author
Juliussen, Brian
Term
4. term
Publication year
2008
Pages
138
Abstract
Hyperglycemia (high blood sugar) is common in critically ill patients and can increase the risk of death. This thesis presents and validates a glycemic control system that uses a physiology-based metabolic model (Glucosafe) together with an integrating-based parameter identification method. The intended use is blood-glucose control in critically ill patients. The system uses the Glucosafe glucose–insulin metabolic model. Each patient’s time-varying insulin sensitivity (SI) is estimated between measurements using an integrating-based method. Performance is assessed by the ability to keep blood glucose in a normoglycemic range of 4.4–7.75 mmol/L. Clinical control interventions are determined by optimization over a set of penalty functions. Validation was carried out on 20 virtual patients built from patient-specific insulin sensitivity profiles derived from clinical data from 20 intensive care patients at Christchurch Hospital (New Zealand). Results show an overall median blood glucose of 6.05 mmol/L (IQR 5.54–6.62 mmol/L), no measurements below 2.2 mmol/L, and an average of 87.7% of measurements within the 4.4–7.75 mmol/L target range. These outcomes are comparable to previous work (Chase et al., 2008) and are acceptable for proceeding to clinical pilot trials.
Hyperglykæmi (forhøjet blodsukker) er almindelig hos kritisk syge og kan øge dødeligheden. Denne afhandling præsenterer og validerer et glykæmisk kontrolsystem baseret på en fysiologisk, modelbaseret tilgang (Glucosafe) samt en integrerende-baseret metode til at identificere modelparametre. Formålet er at styre blodsukkeret hos kritisk syge patienter. Systemet bruger Glucosafe glukose–insulin-metaboliske model. Patienters tidsvarierende insulinfølsomhed (SI) estimeres mellem målinger med en integrerende-baseret metode. Systemets ydelse vurderes ud fra evnen til at holde blodsukker i et normoglykæmisk interval på 4,4–7,75 mmol/L. Kliniske kontrolinterventioner fastlægges ved optimering over en række straffunktioner. Valideringen er udført på 20 virtuelle patienter, baseret på patient-specifikke SI-profiler udledt af kliniske data fra 20 intensivpatienter fra Christchurch Hospital (New Zealand). Resultaterne viser en samlet median blodsukkerkoncentration på 6,05 mmol/L (IQR 5,54–6,62 mmol/L), ingen målinger under 2,2 mmol/L og i gennemsnit 87,7% af målingerne inden for målområdet 4,4–7,75 mmol/L. Disse resultater er på linje med tidligere studier (Chase et al., 2008) og vurderes tilstrækkelige til at gå videre til kliniske pilotforsøg.
[This apstract has been rewritten with the help of AI based on the project's original abstract]
